Why do you need a colposcopy?
Your GP has told you that your cervical screening test (CST) was abnormal and that you need to see a gynaecologist for a colposcopy. What does that mean and what should you expect?
Under the new guidelines, an abnormal CST is one that has returned a positive result for one of the human papillomavirus (HPV) strains that we know can sometimes cause cancer. Depending on which strain of HPV was identified and what the cells looked like under the microscope determines if you need to see a Gynaecologist or if you should simply have your CST repeated in a year. If the HPV is negative then your next CST will be due in five years.
Most importantly, try not to be too anxious about an abnormal CST. It’s designed to pick up changes before they turn into anything significant (like cancer) and the next step in the screening process is to attend an appointment for a colposcopy.
What is a colposcopy?
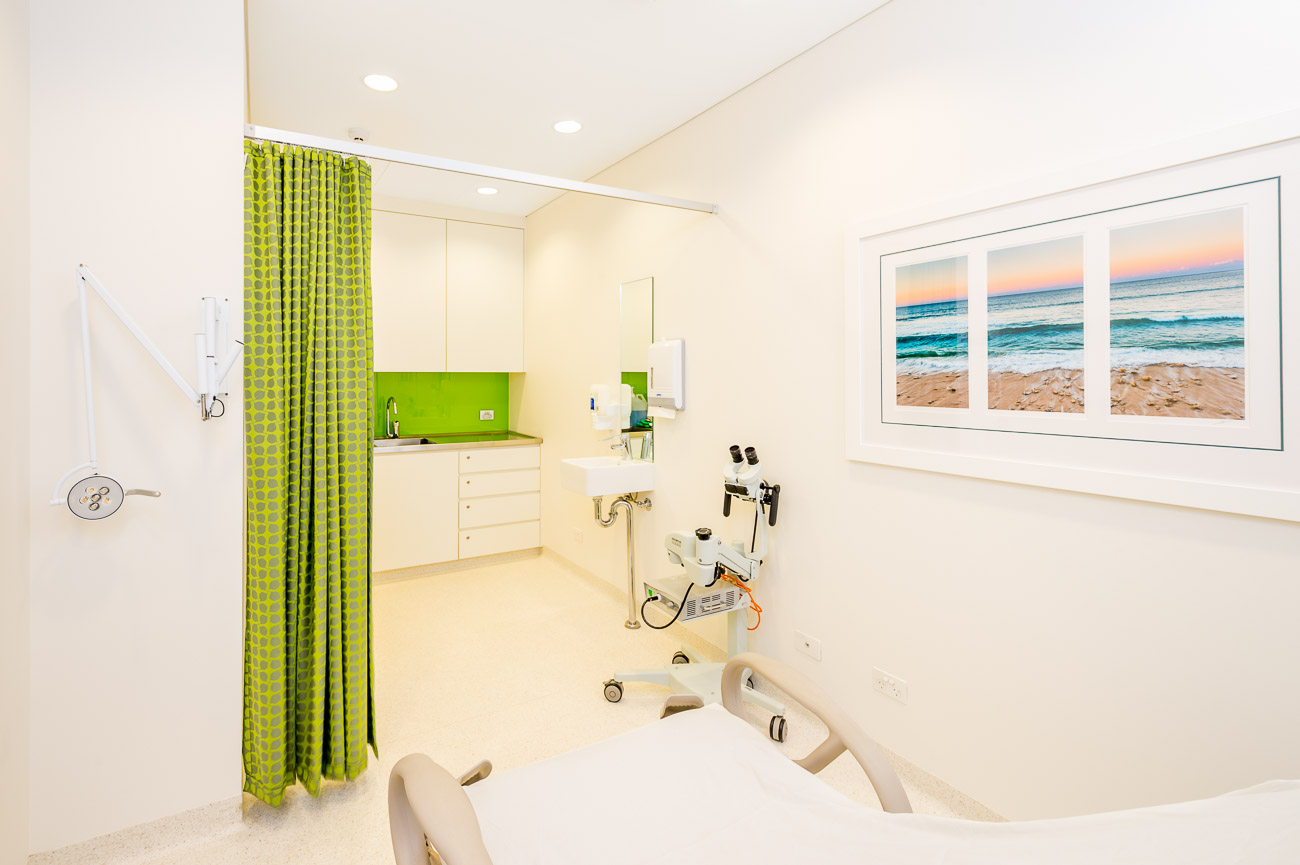
A colposcopy is when a gynaecologist looks at your cervix with a large microscope known as a colposcope – it looks a bit like binoculars on a stand. A special gynaecological bed is used; it has foot rests (a bit like stirrups) and the height of the bed and the back rest are adjustable. Both the bed and the colposcope can be seen in the photograph at the top of this post.
The process is similar to having a cervical screening test, or pap smear. A duckbill speculum is inserted into the vagina and acetic acid (essentially vinegar) is applied to the cervix with large cotton buds. Using the colposcope for magnification, the cervix is assessed for certain patterns and changes that may have occurred. Then Lugol’s iodine is applied to highlight other potential changes.
Sometimes, despite the CST being positive for HPV, the cervix looks completely normal under the microscope. If that is the case, then the colposcopy is complete at that point.
If the cervix looks abnormal, then a biopsy (sample) will be taken of the most abnormal looking areas. A biopsy involves removing a small amount of tissue from the cervix and sending it to a pathologist for further testing. While some women don’t feel the actual biopsy, most women will feel a small pinch. After the biopsy it is very common to experience some crampy pelvic pain, similar to period pain. This usually resolves within a few hours. Any bleeding caused is usually controlled using silver nitrate or Monsell’s solution.
Simple pain relief medications like Paracetamol and Ibuprofen are usually enough to control any discomfort after the biopsy. Increased discharge is common for a few days and it may be quite discoloured due to the substances used to stop the bleeding. It is therefore a good idea to wear a pad or pantyliner for the next few days. Swimming, using tampons, having intercourse and baths should be avoided for about five days after a biopsy due to the risk of infection they present.
The biopsy results are usually available about a week after the colposcopy. You will be contacted with those results and the follow up plan and options for treatment (if required) that were discussed at your appointment will be implemented.